How Fear of Falling Sabotages Recovery After Hip Surgery in Older Adults
As populations around the world age rapidly, healthcare providers and researchers alike grapple with the complex challenges posed by the needs of older adults. One of the most pressing concerns in geriatric medicine is the risk of falling, particularly after hip surgery-a common intervention for injuries such as fractures or degenerative diseases. The consequences of falls in the elderly can be devastating, often leading to prolonged hospital stays, decreased mobility, and significantly impaired quality of life. In a groundbreaking systematic review published in BMC Geriatrics, Ren, Sun, Wu, and colleagues undertook a meticulous sex-specific investigation into the fear of falling following hip surgery, incorporating sophisticated analytical frameworks including GRADE (Grading of Recommendations Assessment, Development, and Evaluation) and PAF (Population Attributable Fraction) assessments to provide an unparalleled depth of understanding on this critical issue.
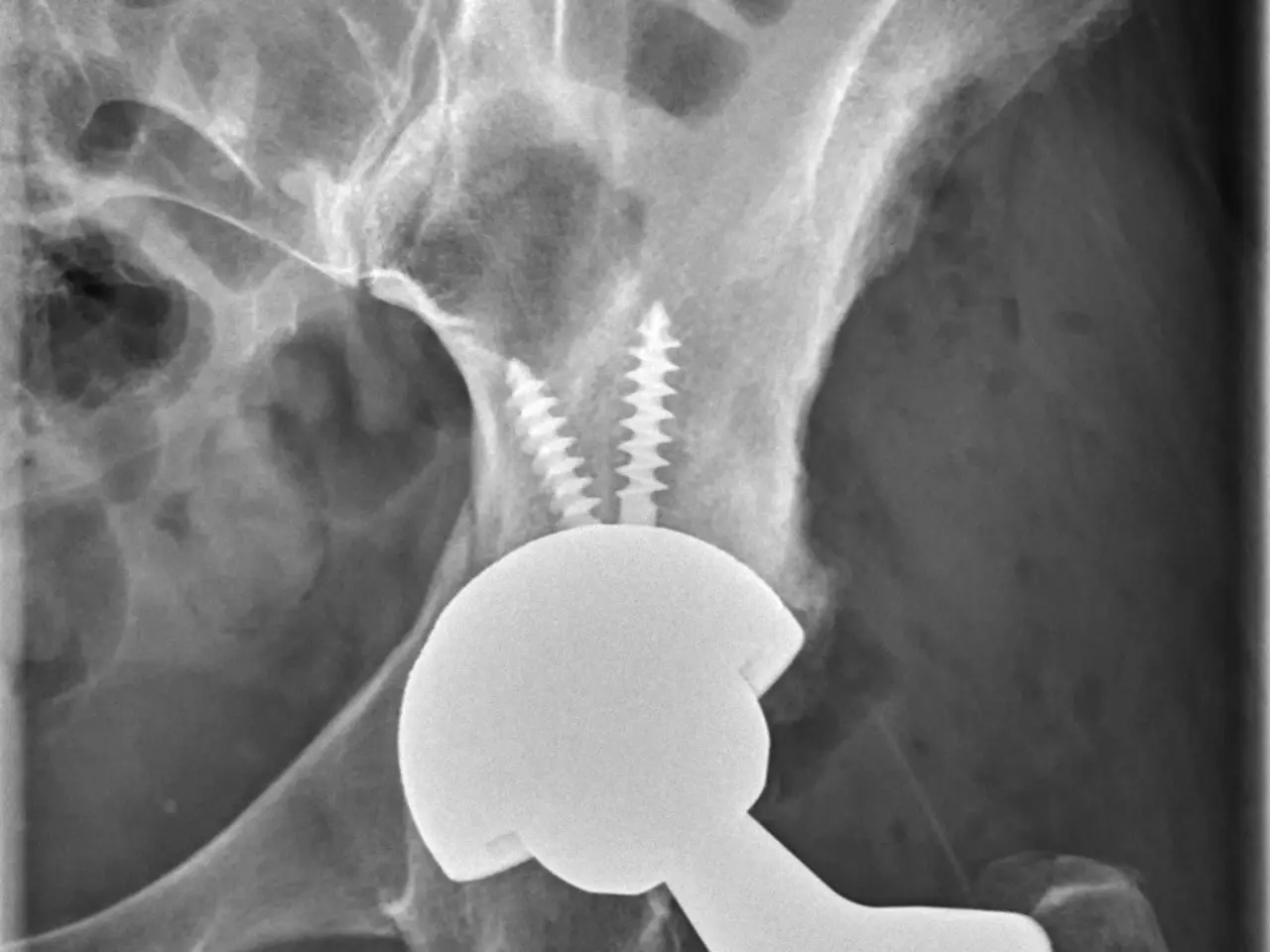
Hip surgery, especially in older individuals, is not simply a procedure but a pivot point in the trajectory of a patient's physical and psychological health. Postoperative recovery transcends the physical repair of bones; it encompasses the restoration of confidence, balance, and independence. Fear of falling-an often under-recognized, yet profoundly impactful psychological consequence-can significantly hamper rehabilitation efforts and lead to a self-perpetuating cycle of inactivity and frailty. The review by Ren and colleagues stands out by differentiating risk profiles between men and women, a dimension frequently overlooked in previous research but essential given the sex-specific physiological and psychosocial factors influencing recovery outcomes.
The systematic review meticulously screened and synthesized data from numerous studies, ensuring that the evidence base was robust and reflective of the latest research advancements. By employing the GRADE framework, the authors were able to critically appraise the quality of evidence, delineating strong recommendations from those supported by moderate or low certainty. This methodological rigor ensures that clinicians can apply these insights with confidence, tailoring interventions to mitigate fear of falling in sex-specific contexts. Additionally, the use of PAF allowed the team to quantify the proportion of fall risk attributable to modifiable factors, highlighting potential targets for targeted prevention strategies.
Diving into the nuances of their findings, the authors reveal that women exhibited a higher propensity to develop fear of falling after hip surgery compared to men. This discrepancy can be traced to a confluence of biological differences, such as variations in muscle mass and bone density, as well as psychological factors including anxiety levels and social support dynamics. The fear of falling, when left unaddressed, often manifests as activity avoidance, which paradoxically increases actual fall risk due to muscle atrophy and diminished balance. For men, while the prevalence was comparatively lower, the psychological consequences were no less significant, underscoring the need for inclusive, gender-sensitive rehabilitation protocols.
Central to the implications of this review is the identification of modifiable risk factors linked to fear of falling. Environmental hazards, poor postoperative pain management, and inadequate psychological support emerged as critical areas of concern. Interventions such as tailored physiotherapy programs, cognitive-behavioral therapy, and home safety assessments are underscored as effective means to break the vicious cycle. Crucially, the review advocates for integrating fear of falling assessments into standard postoperative care pathways, emphasizing early detection and proactive management as pillars to improving patient outcomes.
One particularly striking aspect of the review is its emphasis on the interconnectedness of mental health and physical recovery. The authors argue compellingly that addressing fear of falling should not be siloed from broader efforts to tackle depression, anxiety, and social isolation-conditions that often co-occur in older adults post-surgery. This holistic approach aligns with emerging trends in geriatric medicine that prioritize multidimensional patient care, recognizing that successful rehabilitation hinges not only on physical metrics but also on psychosocial wellbeing.
In clinical practice, the insights derived from this review could transform patient education protocols. Preoperative counseling that includes discussions about fear of falling may prepare patients mentally for the challenges ahead, setting realistic expectations and fostering resilience. Moreover, multidisciplinary teams consisting of orthopedic surgeons, physiotherapists, psychological counselors, and social workers are positioned to deliver comprehensive care tailored to individual patient profiles, optimizing recovery trajectories.
The review further suggests that healthcare systems must adopt sex-specific data tracking and outcome measurements to enhance the precision of future research and intervention design. By establishing sex-disaggregated databases, researchers can continue to elucidate the complex interplay between biological and psychosocial determinants of fear of falling, leading to innovations in personalized medicine for older adults recovering from hip surgery.
Given the global burden of hip fractures and subsequent surgeries, with millions of cases annually, the public health ramifications of these findings are profound. By leveraging the PAF metrics, policymakers and healthcare planners are equipped with quantitative justification to allocate resources towards fall prevention programs, particularly those addressing the psychological dimensions highlighted in this review. Investments in community-based rehabilitation centers, home modification initiatives, and caregiver training programs emerge as cost-effective strategies aligned with the evidence presented.
Importantly, the review also highlights gaps and future directions for research. The heterogeneity in study designs and outcome measures across the included literature underscores the need for standardized protocols in fear of falling research. Future work could explore innovative technologies such as wearable sensors to objectively monitor balance and movement, thereby refining assessments and tailoring interventions in real-time. Moreover, longitudinal studies tracking long-term outcomes beyond the immediate postoperative period would shed light on the durability of prevention strategies and the evolving nature of fear of falling with aging.
The interdisciplinary nature of this systematic review bridges orthopedics, geriatrics, psychology, and public health, exemplifying the collaborative spirit necessary to tackle complex geriatric syndromes. By foregrounding the sex-specific dimensions of fear of falling, Ren and colleagues not only advance scientific knowledge but also chart a pragmatic course for improving the lives of countless older adults worldwide. Their work serves as a clarion call to reimagine postoperative care through a more nuanced, empathetic lens, recognizing fear of falling as a critical, modifiable determinant of recovery.
In conclusion, this seminal review underscores that fear of falling after hip surgery is not merely an isolated fear but a multifaceted syndrome demanding urgent attention. Its implications extend beyond individual patients to families, healthcare systems, and societies at large. The intersectional insights provided pave the way for more effective, personalized interventions-ushering in a new era of geriatric care that holistically addresses the physical and psychological aftermath of hip surgery. As populations continue to age, integrating these findings into clinical practice could markedly reduce fall rates, enhance quality of life, and ultimately transform the narrative surrounding aging and mobility.