Late-night habits linked to higher emotional instability, study reveals
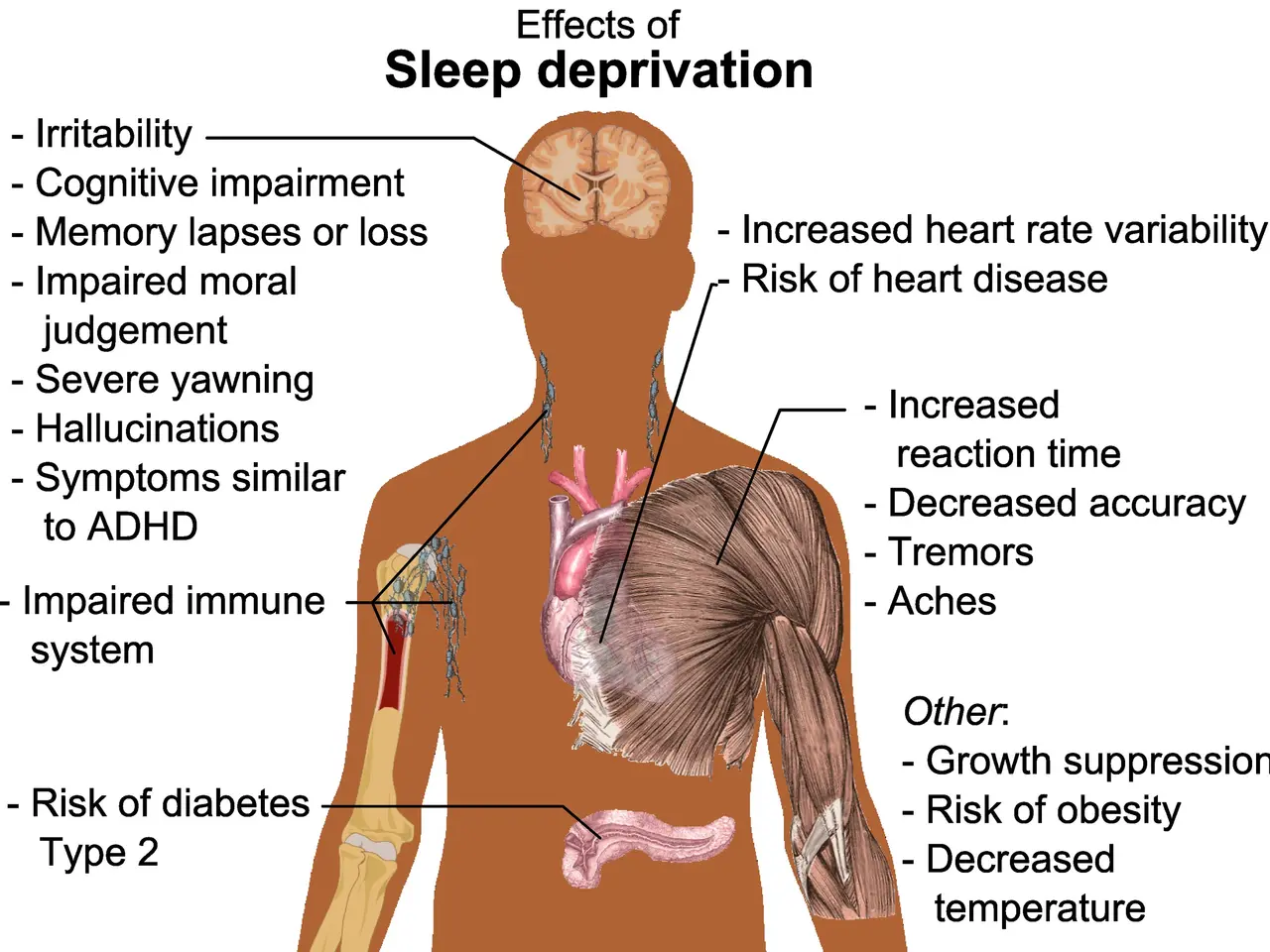
A new study has uncovered a clear link between sleep patterns and emotional health. Researchers analysed data from over 2,000 Italian adults to explore how natural sleep preferences—whether someone is a morning person, evening person, or neither—affect mood and mental well-being. The findings suggest that those who stay up late face greater risks of emotional instability and mood-related vulnerabilities. The study involved 2,031 adults, with 22.8% identifying as evening types, 22.2% as morning types, and the remaining 55% as neutral. Participants classified as evening chronotypes showed significantly higher levels of emotional dysregulation compared to morning and neutral types. They also scored higher on measures of depressive, anxious, irritable, and cyclothymic temperaments—traits often linked to bipolar vulnerability.
Further analysis revealed that evening chronotypes had elevated scores on the Mood Disorder Questionnaire (MDQ) and the Hypomania Checklist (HCL-32-R2). These results indicate a stronger association with subthreshold bipolar features. Among all factors examined, only evening chronotype and tobacco use remained significant predictors of these mood patterns in deeper statistical models. The research also highlighted protective factors. Good or excellent sleep quality appeared to reduce the risk of developing subclinical bipolar traits. In response, psychiatrists recommend structured interventions to stabilise daily rhythms. These include fixed sleep schedules, regular meal and work routines, mood tracking, and therapies like interpersonal and social rhythm therapy (IPSRT). Medication timing, such as evening sedatives, is often combined with these strategies to reinforce consistency. In practice, these approaches are delivered through patient education, cognitive behavioural therapy (CBT), and ongoing monitoring with mood calendars. The goal is to prevent episode worsening by maintaining steady biorhythms—particularly critical for evening types, whose disrupted sleep-wake cycles heighten vulnerability.
The findings underscore the importance of sleep patterns in mental health, especially for those with a late-night preference. With roughly one in three UK adults identifying as 'night owls,' the study suggests targeted interventions could help mitigate emotional dysregulation risks. Clinicians now advocate for routine sleep assessments and personalised rhythm-stabilising strategies to support long-term mood stability.