Who hasn't been there: You lie in bed, your body exhausted, but your mind racing at full speed. Or you drift off to sleep, only to wake up after a few hours and struggle to fall back asleep. What may sound like an occasional nuisance has long become a daily reality for millions in Germany—with noticeable consequences for concentration, mood, and physical health.
Sleep disorders are among the most underestimated health problems of our time. Yet the numbers speak for themselves: Around a quarter of the adult population in Germany regularly suffers from difficulty falling or staying asleep, according to estimates. The actual figure is likely even higher, as many people seek medical help late—or not at all.
Why sleep disorders have become so common
Germany's sleep crisis deepens as one in four adults battles insomnia
The reasons behind the rising prevalence of sleep disorders are diverse and often interconnected. Chronic stress in both professional and personal life plays a central role. When the nervous system remains in a constant state of alert, the body struggles to shift into rest mode—even when we want it to.
Add to that our changed relationship with light and time. Screens used right up until bedtime suppress the production of melatonin, the body's natural sleep hormone. Irregular working hours, shift work, and so-called "social jet lag"—the mismatch between our biological clock and societal schedules—further strain our sleep-wake system.
Societal factors also contribute. The expectation of constant availability, the flood of information, and a cultural climate that prioritizes productivity over recovery have turned sleep into an afterthought for many—something left over only after everything else is done.
The toll of poor sleep in daily life
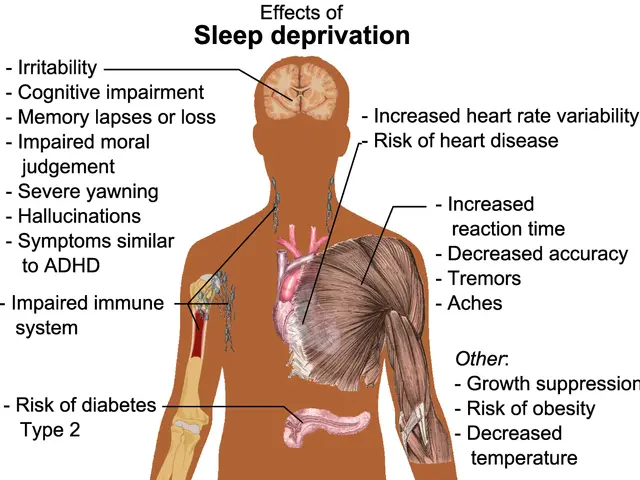
The effects of chronic sleep disruption are profound. In the short term, concentration wanes, reaction times slow, and emotional resilience weakens. Those who regularly sleep too little or poorly become more irritable, prone to conflict, and perceive stress more intensely.
Over the medium and long term, the consequences grow more serious and demand medical attention. According to the German Society for Sleep Research and Sleep Medicine, persistent sleep disorders are closely linked to an increased risk of cardiovascular diseases, metabolic disorders such as type 2 diabetes, and mental health conditions, particularly depression and anxiety. Sleep is not passive downtime but an active phase of regeneration—when the brain processes information, the immune system recovers, and cells renew themselves.
The most common types of sleep disorders
Not all sleep disorders are the same. Medicine distinguishes between different forms, each with distinct causes and requiring different treatments.
The most common is insomnia: sufferers struggle to fall asleep, wake frequently, or rise too early, leaving them unrefreshed despite spending enough time in bed. Separate from this is sleep apnea, characterized by breathing interruptions during the night—often unnoticed by those affected but leaving them exhausted and drowsy by day. Restless legs syndrome, where uncomfortable sensations in the legs disrupt sleep, along with sleepwalking or nocturnal panic attacks, complete the picture.
When should poor sleep be treated?
Occasional sleep problems—such as during stressful periods or after major life events—are normal and usually resolve on their own. However, it becomes critical when sleep disturbances persist for more than three weeks, occur at least three times a week, and noticeably impair daily functioning.
At this stage, medical guidelines recommend seeking professional advice. The longer sleep disorders go untreated, the more entrenched they become—both physiologically and psychologically. What may begin as a situational sleep issue can develop into chronic insomnia, which rarely disappears without targeted intervention.
What Really Works: Proven Approaches to Better Sleep
Cognitive behavioral therapy for insomnia (CBT-I) is now the gold standard for treating chronic insomnia. Research shows that this form of therapy is more effective in the long term than sleep medications, without causing dependence or tolerance. The focus lies on identifying disruptive thought patterns, modifying sleep habits, and applying targeted techniques such as sleep restriction and stimulus control.
Complementary sleep hygiene measures can also make a difference: maintaining consistent bedtimes and wake-up times, keeping the bedroom cool and dark, avoiding screens in the hours before bed, and mindfully managing caffeine and alcohol intake.
While sleep medications may be useful in certain short-term situations, they are not a sustainable solution. Many only address symptoms, disrupt natural sleep architecture, and can lead to dependence with prolonged use.
New Paths to Treatment: Current Shifts in Sleep Therapy
The landscape of sleep disorder treatment has evolved significantly in recent years. Alongside traditional therapies, more individualized and accessible approaches—such as telemedicine and digital therapy programs—are gaining traction.
Medical cannabis therapy is also receiving greater attention in this context. For certain patients who do not respond adequately to conventional treatments, cannabis under medical supervision may become part of a holistic therapy plan. People with comorbid conditions, such as chronic pain or severe anxiety disorders, often report improved sleep as a result.
Conclusion: Good Sleep Isn't a Luxury—It's Essential
Sleep disorders are not a sign of weakness or a lifestyle issue. They represent a serious health challenge that, with consistent treatment, can often be significantly improved. Anyone experiencing persistent poor sleep should take action rather than waiting.
The first step is often the simplest: a conversation with a doctor. Prioritizing sleep is an investment in nearly every other aspect of health.
This article is for general informational purposes only and does not replace professional medical advice.