New Depression Therapy Targets Anhedonia by Rebuilding Brain's Reward System
For decades, the mental health field has operated on a half-truth: that curing depression means removing sadness. A new study argues that the most dangerous part of depression isn't negative emotion, it's the absence of positive emotion, known as anhedonia.
Affecting 90% of patients, anhedonia is a primary predictor of suicide and chronic illness. The researchers have introduced Positive Affect Treatment (PAT), a 15-session therapy that ignores 'fixing' sadness and instead focuses exclusively on rebuilding the brain's capacity for joy, motivation, and reward.
The Treatment Gap: Conventional therapies focus on reducing negative symptoms (anxiety, sadness, fear). PAT shifts the focus to 'positive affect,' targeting the brain's reward system directly.
Paradoxical Healing: In clinical trials, patients who received PAT improved in both positive and negative measures, even though negative emotions were never addressed during the sessions.
Hopelessness vs. Helplessness: Lead researcher Alicia E. Meuret distinguishes between the two: 'Helplessness' still contains a drive to change; 'Hopelessness' (anhedonia) is the belief that nothing can change.
The Power of Savoring: PAT utilizes specific exercises like 'savoring,' gratitude, and loving-kindness to retrain how the brain anticipates and learns from rewarding events.
Superior Outcomes: In a trial of 98 adults, PAT outperformed conventional therapies in overall clinical status, proving more effective at reducing suicidal behavior and relapse risks.
Most people know depression as a disorder of sadness. But for millions of patients, the most debilitating feature is something else entirely: the reduced ability or inability to feel positive emotions.
Anhedonia affects nearly 90% of people with major depression. It predicts a longer, more severe course of illness, undermines recovery and is a substantial predictor of suicidal behavior. Anhedonia also appears in anxiety disorders, PTSD, substance use disorders and schizophrenia, yet most conventional treatments do not address it.
For decades, treatment has focused almost entirely on reducing negative emotions, leaving anhedonia largely unaddressed. Patients themselves actually view restoring positive emotion as their primary goal, even more than reducing negative symptoms.
A new study in JAMA Network Open by SMU psychologists Alicia E. Meuret and Thomas Ritz and Michelle G. Craske at UCLA suggests targeting positive emotions directly is a more powerful treatment approach. The research is the culmination of more than a decade of clinical trials examining Positive Affect Treatment, or PAT, a 15-session psychotherapy designed to rebuild patients' capacity for joy, purpose, motivation and reward.
'There's a difference between feeling helpless and feeling hopeless,' said Meuret, who leads the Anxiety and Depression Research Center at SMU. 'When you feel helpless, you still have the drive and the will to want to change things. When people feel hopeless, they don't believe anything will change. That's what anhedonia can look like, and taking away negative emotions doesn't fix it.'
Targeting the brain's reward system
PAT was developed to directly target the brain's reward system, which governs how people anticipate, experience, and learn from positive events. The therapy retrains what researchers describe as the brain's 'positive system' through exercises that re-engage patients with rewarding activities, redirect attention toward positive experiences, and build practices such as gratitude, savoring, and loving-kindness.
Unlike conventional treatments that address negative emotions directly, PAT focuses exclusively on positive affect. That distinction makes its results more striking: patients improved on both positive and negative measures despite the treatment never targeting negativity at all.
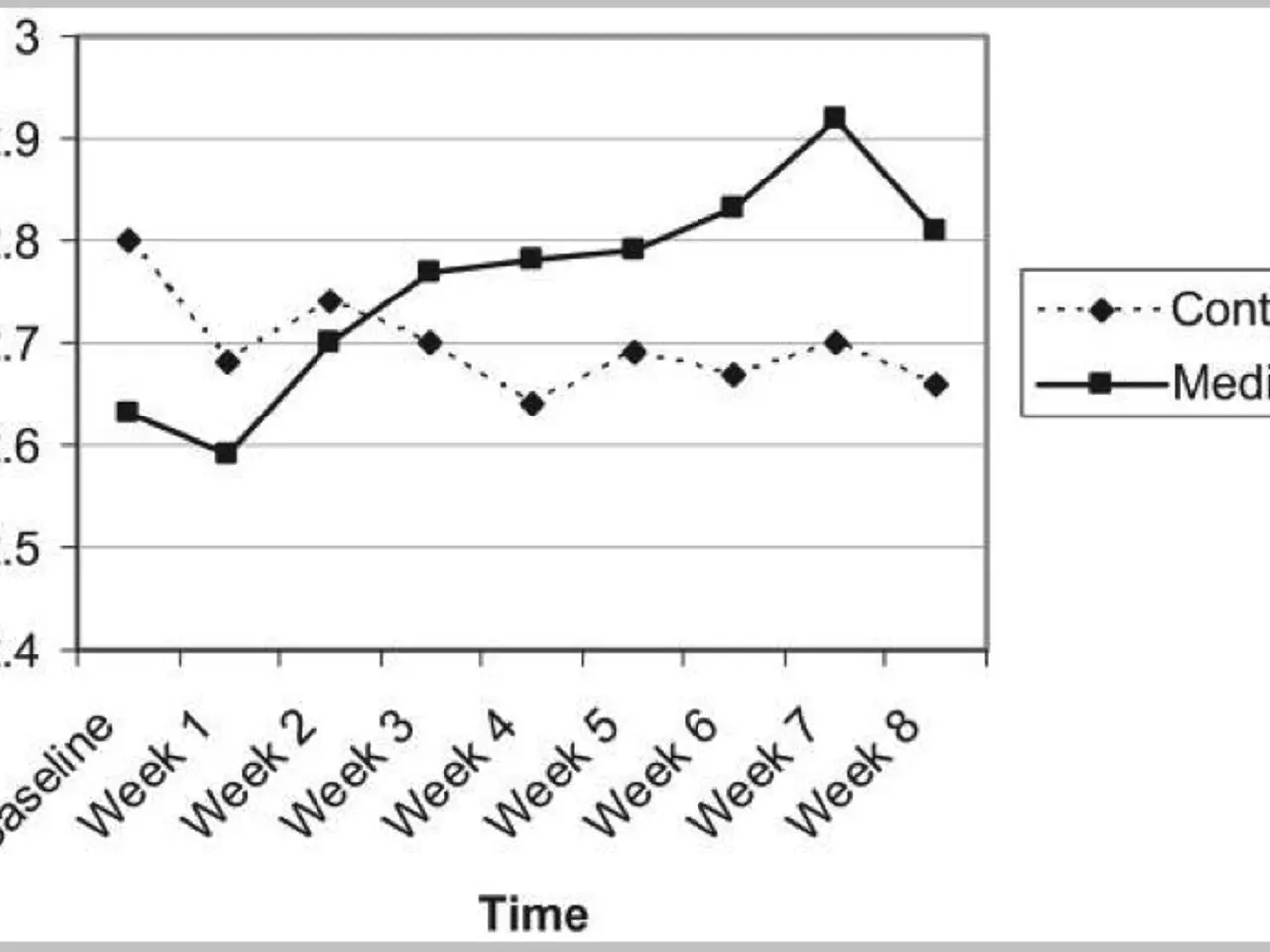
In a randomized controlled trial of 98 adults with severe anhedonia, depression and anxiety, PAT produced greater improvements in overall clinical status than a conventional therapy targeting negative affect, an advantage that held at one-month follow-up.
Patients also showed significant reductions in depression and anxiety symptoms. Researchers identified modulation of reward and threat processes as a central mechanism driving those gains.
Reducing key risk factors in depression and anxiety
Targeting impaired reward processing, the researchers concluded, is essential for reducing key risk factors in depression and anxiety, including suicidality and relapse.
'It's not enough to take away the bad,' Meuret said. 'Treatment needs to ask: Is this activity meaningful to you? Will it give you joy or a sense of accomplishment? Does it foster connection?'
The study used 9 measures to track changes in reward sensitivity across three domains: reward anticipation and motivation, response to reward attainment, and reward learning, in addition to 5 threat processing measures, drawn from self-report, behavioral tasks, and physiological assessments. Six of seven self-reported reward and threat measures mediated clinical outcomes. Behavioral and physiological measures did not show the same effect.
Key Questions Answered:
Q: Why doesn't 'taking away the bad' automatically make me feel good?
A: Negative and positive emotions aren't two sides of a single see-saw; they are controlled by different systems in the brain. You can stop a car from sliding backward (removing negative affect) without ever putting it in 'drive' (activating the positive system).
Q: How do you 'retrain' a brain that physically can't feel joy?
A: PAT uses reward learning. By repeatedly engaging in meaningful activities and intentionally 'savoring' even tiny positive moments, patients can slowly rebuild the neural pathways that govern anticipation and motivation. It's like physical therapy for the brain's reward center.
Q: Does this mean we should stop treating anxiety and sadness?
A: No, but it means we should stop treating them as the only goals. For patients with severe anhedonia, restoring a sense of accomplishment and connection is often the only way to break the cycle of 'hopelessness' that leads to long-term disability and suicide.